Formulary Exception Form
Formulary Exception Form - By checking this box and signing below, i certify that applying the standard review time frame may seriously jeopardize the life or health of the patient or the patient’s ability to regain maximum function. Your doctor can go online and request a coverage decision for you. The documents accompanying this transmission contain confidential health information that is legally privileged. This form is for prospective, concurrent, and retrospective reviews. Web a formulary exception should be requested to obtain a part d drug that is not included on a plan sponsor's formulary, or to request to have a utilization management requirement waived (e.g., step therapy, prior authorization, quantity limit) for a. Web formulary exception request form formulary exception request this form may be used to request exceptions from the drug formulary, including drugs requiring prior authorization. Web formulary exception/prior authorization request form expedited/urgent review requested: Please note that the prescription benefit and/or plan contract may exclude certain medications. Incomplete forms will be returned for additional information. Web formulary exception prior authorization/medical necessity determination prescriber fax form only the prescriber may complete this form.
Web when faced with uncovered medications, you have an option to file a formulary exception with your insurance to request that they allow you coverage for the medication. Web formulary exception/prior authorization request form expedited/urgent review requested: Select the list of exceptions for your plan. By checking this box and signing below, i certify that applying the standard review time frame may seriously jeopardize the life or health of the patient or the patient’s ability to regain maximum function. Web a formulary exception should be requested to obtain a part d drug that is not included on a plan sponsor's formulary, or to request to have a utilization management requirement waived (e.g., step therapy, prior authorization, quantity limit) for a. Your doctor can go online and request a coverage decision for you. Please note that the prescription benefit and/or plan contract may exclude certain medications. This form is for prospective, concurrent, and retrospective reviews. The documents accompanying this transmission contain confidential health information that is legally privileged. Web formulary exception prior authorization/medical necessity determination prescriber fax form only the prescriber may complete this form.
Web a formulary exception should be requested to obtain a part d drug that is not included on a plan sponsor's formulary, or to request to have a utilization management requirement waived (e.g., step therapy, prior authorization, quantity limit) for a. Web complete this form to request a formulary exception, tiering exception, prior authorization or reimbursement. Most plans require that your doctor submit a. Web formulary exception request form formulary exception request this form may be used to request exceptions from the drug formulary, including drugs requiring prior authorization. Web request rationale history of a medical condition, allergies or other pertinent information requiring the use of this medication: Web when faced with uncovered medications, you have an option to file a formulary exception with your insurance to request that they allow you coverage for the medication. Web formulary exception/prior authorization request form expedited/urgent review requested: Start saving time today by filling out this prior. Web formulary exception prior authorization/medical necessity determination prescriber fax form only the prescriber may complete this form. Web formulary exception requests will be evaluated and a determination of coverage made utilizing all the following criteria:
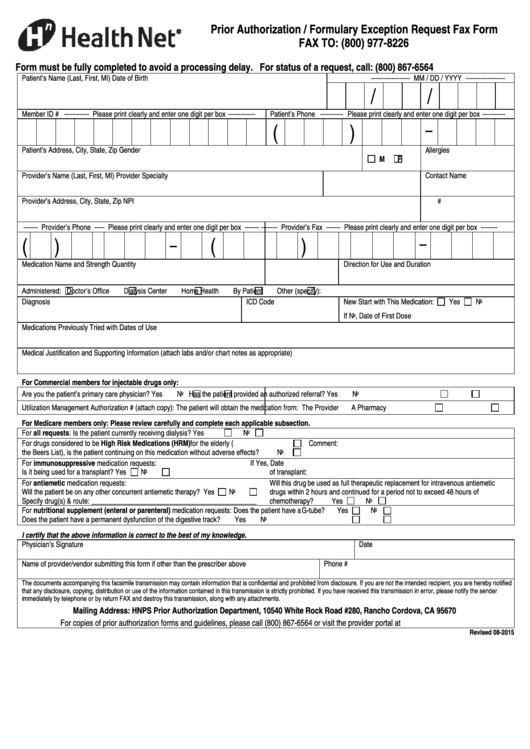
Health Net Prior Authorization / Formulary Exception Request Fax Form
Web formulary exception/prior authorization request form expedited/urgent review requested: Web formulary exception prior authorization/medical necessity determination prescriber fax form only the prescriber may complete this form. Web when faced with uncovered medications, you have an option to file a formulary exception with your insurance to request that they allow you coverage for the medication. Web complete this form to request.
Bcbs Formulary Exception Form Fill Online, Printable, Fillable, Blank
Web complete this form to request a formulary exception, tiering exception, prior authorization or reimbursement. Web formulary exception prior authorization/medical necessity determination prescriber fax form only the prescriber may complete this form. Web when faced with uncovered medications, you have an option to file a formulary exception with your insurance to request that they allow you coverage for the medication..
Form Frx004 Formulary Exception Request Form printable pdf download
Member’s eligibility to receive requested services (enrollment in the plan, prescription drug coverage, specific exclusions in member’s contract) The documents accompanying this transmission contain confidential health information that is legally privileged. Most plans require that your doctor submit a. Web request rationale history of a medical condition, allergies or other pertinent information requiring the use of this medication: Web when.
Form Frx001 Tier Exception Request Form printable pdf download
Please note that the prescription benefit and/or plan contract may exclude certain medications. Web formulary exception prior authorization/medical necessity determination prescriber fax form only the prescriber may complete this form. Web request rationale history of a medical condition, allergies or other pertinent information requiring the use of this medication: Incomplete forms will be returned for additional information. Web when faced.
FORMULARY EXCEPTION PHYSICIAN FAX FORM Fill Out and Sign Printable
The documents accompanying this transmission contain confidential health information that is legally privileged. Web request rationale history of a medical condition, allergies or other pertinent information requiring the use of this medication: Select the list of exceptions for your plan. Web formulary exception requests will be evaluated and a determination of coverage made utilizing all the following criteria: Start saving.
New York Prior Approval/Nonformulary Medication Request Form Blue
Incomplete forms will be returned for additional information. Web request rationale history of a medical condition, allergies or other pertinent information requiring the use of this medication: By checking this box and signing below, i certify that applying the standard review time frame may seriously jeopardize the life or health of the patient or the patient’s ability to regain maximum.
Sample Prime Therapeutics Prior Authorization Form Sample Templates
Web formulary exception requests will be evaluated and a determination of coverage made utilizing all the following criteria: Your doctor can go online and request a coverage decision for you. Web when faced with uncovered medications, you have an option to file a formulary exception with your insurance to request that they allow you coverage for the medication. Web formulary.
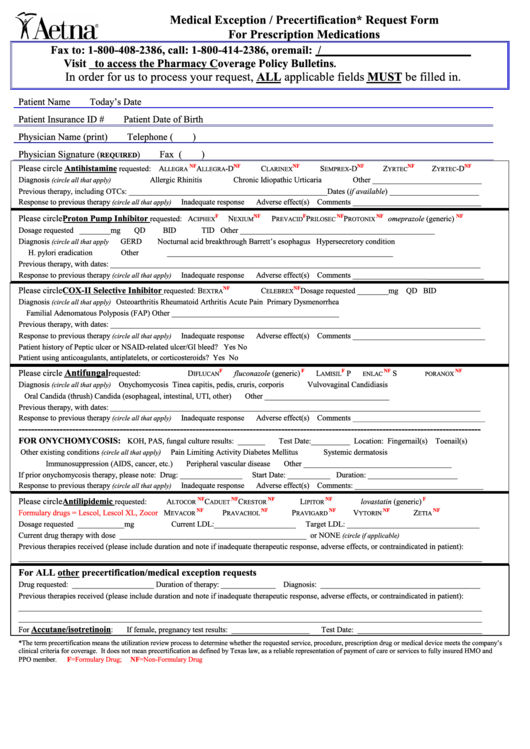
Aetna Medical Exception / Precertification Request Form printable pdf
Web formulary exception request form formulary exception request this form may be used to request exceptions from the drug formulary, including drugs requiring prior authorization. Web formulary exception prior authorization/medical necessity determination prescriber fax form only the prescriber may complete this form. Please note that the prescription benefit and/or plan contract may exclude certain medications. Web complete this form to.
Anthem Medicare Advantage Disenrollment Form Form Resume Examples
Web when faced with uncovered medications, you have an option to file a formulary exception with your insurance to request that they allow you coverage for the medication. Web complete this form to request a formulary exception, tiering exception, prior authorization or reimbursement. This form is for prospective, concurrent, and retrospective reviews. Web formulary exception prior authorization/medical necessity determination prescriber.
Form Frx002 Expedited Formulary Exception Request Form printable pdf
This form is for prospective, concurrent, and retrospective reviews. Web when faced with uncovered medications, you have an option to file a formulary exception with your insurance to request that they allow you coverage for the medication. The documents accompanying this transmission contain confidential health information that is legally privileged. Most plans require that your doctor submit a. Web a.
Most Plans Require That Your Doctor Submit A.
Web when faced with uncovered medications, you have an option to file a formulary exception with your insurance to request that they allow you coverage for the medication. Web formulary exception request form formulary exception request this form may be used to request exceptions from the drug formulary, including drugs requiring prior authorization. Incomplete forms will be returned for additional information. Web complete this form to request a formulary exception, tiering exception, prior authorization or reimbursement.
Please Note That The Prescription Benefit And/Or Plan Contract May Exclude Certain Medications.
Web formulary exception prior authorization/medical necessity determination prescriber fax form only the prescriber may complete this form. Web formulary exception/prior authorization request form expedited/urgent review requested: This form is for prospective, concurrent, and retrospective reviews. Select the list of exceptions for your plan.
Start Saving Time Today By Filling Out This Prior.
Web a formulary exception should be requested to obtain a part d drug that is not included on a plan sponsor's formulary, or to request to have a utilization management requirement waived (e.g., step therapy, prior authorization, quantity limit) for a. The documents accompanying this transmission contain confidential health information that is legally privileged. By checking this box and signing below, i certify that applying the standard review time frame may seriously jeopardize the life or health of the patient or the patient’s ability to regain maximum function. Web request rationale history of a medical condition, allergies or other pertinent information requiring the use of this medication:
Your Doctor Can Go Online And Request A Coverage Decision For You.
Member’s eligibility to receive requested services (enrollment in the plan, prescription drug coverage, specific exclusions in member’s contract) Web formulary exception requests will be evaluated and a determination of coverage made utilizing all the following criteria: